For practically three years, Eric Tennant endured chemotherapy infusions, rounds of radiation, biopsies, and hospitalizations that left him weak and depleted.
“It’s good to be dwelling,” he mentioned after one hospital keep in early June, “but I’m drained and able to get on with issues.”
In 2023, Tennant, of Bridgeport, West Virginia, was recognized with cholangiocarcinoma, a uncommon most cancers of the bile ducts that had unfold all through his physique.
Not one of the preliminary therapies prescribed by his medical doctors had eradicated the most cancers. However a glimmer of hope got here in early 2025, when Tennant was advisable for histotripsy, a comparatively new process that might use ultrasound waves to focus on, and doubtlessly destroy, the most important tumor in his physique — in his liver.
“My dad was somewhat nervous as a result of it was one thing new, nevertheless it positively gave us some hope that he could be round somewhat bit longer,” mentioned Tennant’s daughter, Amiya.
There was only one hitch: His insurer wouldn’t pay for it.
Tennant, 58, died of most cancers on Sept. 17. His story illustrates how a bureaucratic course of referred to as prior authorization can devastate sufferers and their households.
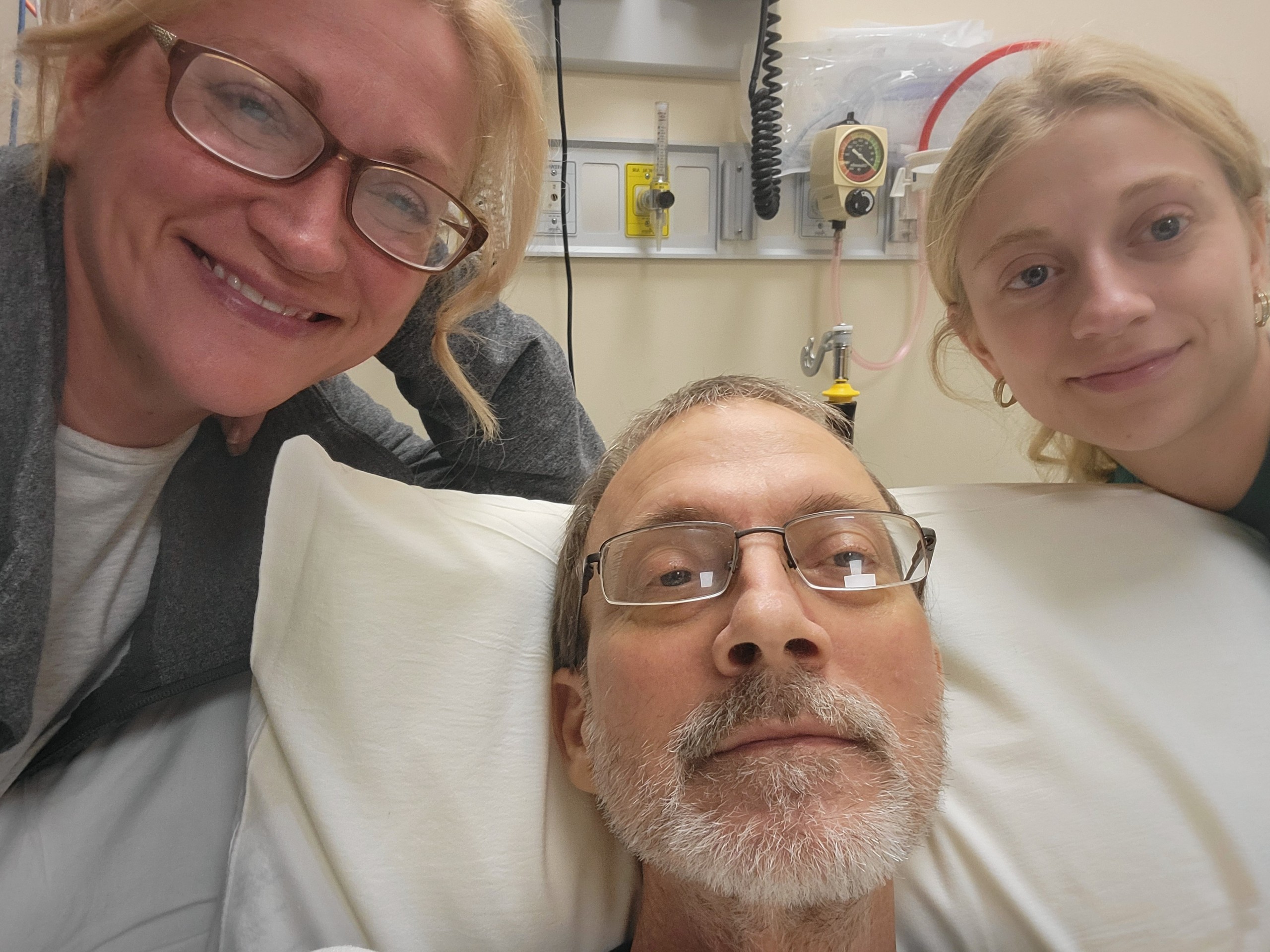
Becky Tennant thinks her husband might need lived longer if their well being insurer had not repeatedly denied a brand new remedy advisable by his physician early this 12 months. “It could not have modified the end result,” she says, “however they took that away from us to know.” (Rebecca Tennant)

For months, Eric Tennant’s well being insurer refused to cowl a most cancers remedy advisable by his physician, claiming the process was “not medically mandatory,” a standard motive utilized by insurers to disclaim care. (A portion of this photograph is digitally blurred to guard affected person privateness.) (NBC Information)
It’s infeasible to depend the folks harmed by this overwhelmingly unpopular followwhich, by delaying or denying care, helps drive well being insurers’ earnings. No authorities company or non-public group tracks such information.
That mentioned, KFF Well being Information has heard from lots of of sufferers in recent times who declare that they or somebody of their household has been harmed by prior authorization. Greater than 1 in 4 physicians surveyed by the American Medical Affiliation in December mentioned that prior authorization had led to a critical opposed occasion for a affected person of their care. And eight% responded that prior authorization led to a incapacity, start defect, or loss of life.
In June, the Trump administration introduced a pledgesigned by dozens of personal insurers, to streamline prior authorization, which regularly requires sufferers or their medical groups to ask insurers for permission earlier than continuing with many forms of care. It stays unclear when sufferers can count on to see enchancment.
The commitments “depend upon the total cooperation of the non-public insurance coverage sector” and can “take time to realize their full impact,” mentioned Andrew Nixon, a spokesperson for the Division of Well being and Human Providers. However the pledge exists, he mentioned, “to forestall tragic deaths like Eric’s from occurring by the hands of an inefficient system.”
Chris Bond, a spokesperson for AHIP, a medical health insurance business commerce group, mentioned he couldn’t communicate to any particular insurer’s prior authorization insurance policies. Broadly, although, he mentioned prior authorization “acts as a guardrail” to verify medicines and coverings should not used inappropriately.
On the similar time, he mentioned, insurers acknowledge that sufferers could be annoyed when their doctor-recommended care is denied. That’s why “there’s a devoted effort throughout the business to make the method extra simple, sooner, and less complicated for sufferers and suppliers,” Bond mentioned.
Within the meantime, the method continues to take its toll on folks like Eric Tennant, whose grave diagnoses typically require costly well being care providers.
“Eric is gone,” his widow, Becky, mentioned. “He’s not coming again.”

Tennant was a security teacher for the West Virginia Workplace of Miners’ Well being Security and Coaching and insured by the state’s Public Workers Insurance coverage Company, which contracts with UnitedHealthcare to manage advantages for state staff, their spouses, and dependents.
In February and March, UnitedHealthcare, the Public Workers Insurance coverage Company, and an outdoor reviewer issued a collection of denials that concluded Eric’s advantages wouldn’t cowl histotripsy, claiming the remedy was not medically mandatory. Becky Tennant estimated the process would price the household about $50,000 out-of-pocket.
Though the remedy wasn’t assured to work, it was price a shot, the Tennants thought, so that they thought of withdrawing cash from their retirement financial savings. However then, in Might, after KFF Well being Information and NBC Information posed a collection of inquiries to UnitedHealthcare and the Public Workers Insurance coverage Company about Eric’s case, the company reversed course. PEIA determined to cowl his remedy.
Notably, the company contacted KFF Well being Information in regards to the approval hours earlier than it notified the Tennant household of the choice.
However the approval got here too late. Eric was hospitalized in late Might and prescribed remedy that prevented him from present process histotripsy at the moment. His household held out hope that his well being would enhance and he would qualify for the process that summer time.
In July, they took a household trip to Marco Island, Florida. It will be their final. Two days after they returned dwelling, a scan revealed Eric’s most cancers had continued to unfold. Histotripsy was out of the query.

“I’m unhappy for what we’ll miss out on,” Becky mentioned. “I’m unhappy on the unfairness of it.”
She mentioned if Eric had been in a position to bear histotripsy in February, as initially advisable by his physician, it might need destroyed the tumor in his liver that in the end killed him.
“We’ll by no means know. That’s the factor. Any lawyer for the insurance coverage will say, ‘Effectively, you don’t know it will have helped.’ No. You took that probability away from us,” she mentioned.
In October, Samantha Knapp, a spokesperson for the West Virginia Division of Administration, instructed KFF Well being Information that the Public Workers Insurance coverage Company has not modified its insurance policies associated to prior authorization for histotripsy and continues to comply with UnitedHealthcare’s pointers.
UnitedHealthcare declined to reply questions for this text.
On Sept. 17, in a hospice mattress arrange of their eating room, Eric was surrounded by his household and their canines as he died. Becky held his hand as his coronary heart fee started to drop.
“He wasn’t afraid to die, however he didn’t wish to die,” she mentioned. “And you would inform the final day that he was preventing it huge time.”
On the very finish, she whispered in his ear: “ I like you. You will have been one of the best husband and one of the best dad, and also you’ve all the time taken such excellent care of us,” Becky recalled.
After which, she mentioned, he gasped. His eyebrows appeared to shoot up in marvel. Throughout his final second alive, she mentioned, he smiled.
“The look on his face was pure, complete amazement,” she mentioned. “I nonetheless can’t consider he’s not right here.”

Do you might have an expertise with prior authorization you’d prefer to share? Click on right here to inform KFF Well being Information your story.

